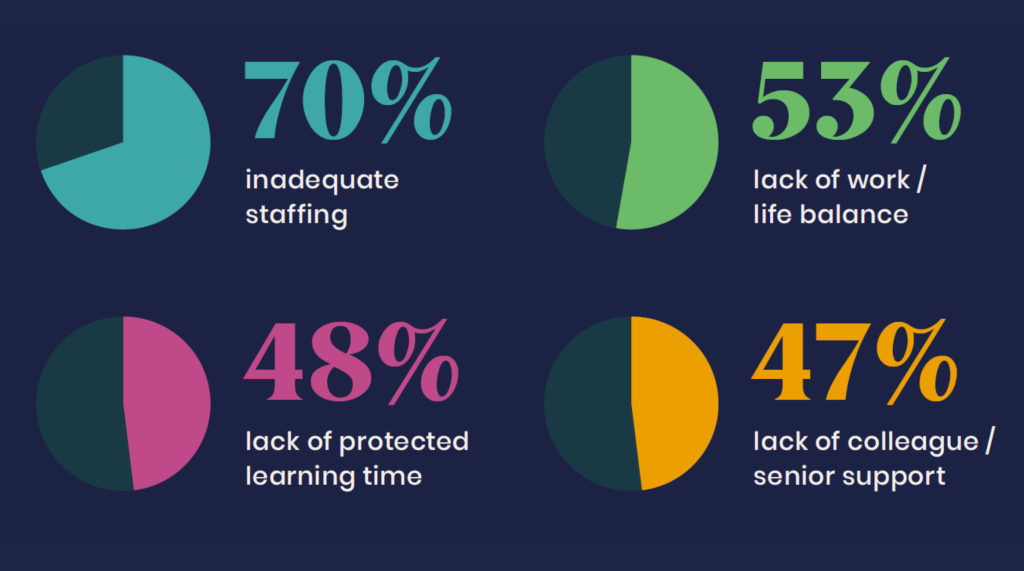
Community respondents were also more likely to rate their mental health as poor (45%) compared to the average (37%) and be less likely to be offered protected learning time (5% vs an average 22%). A higher number of respondents working in community pharmacy (20%) reported not being offered breaks compared to all other sectors (8%) and were more likely to experience verbal or physical abuse from patients and the public (69% vs an average 44%).
Tools, training and support for pharmacy leaders
“For the fourth year running this report exposes some disturbing statistics” commented Danielle Hunt, Chief Executive of Pharmacist Support. “The state of mental health and wellbeing in pharmacy is a huge concern, with the risk of burnout of those working within the profession remaining worryingly high.
“As the profession’s independent charity focused on wellbeing, the results of this report echo many of the individual stories we hear from those who come to the charity for support. During the past year we have experienced a large increase in the number of people reaching out for counselling and looking to share their own experiences with mental health and wellbeing via our ACTNow campaign. Our 2022 campaign concentrated on opening conversations, aiding understanding, exposing barriers and beginning to address workplace culture issues in order to remove the stigma associated with mental health in pharmacy.
“The survey results also highlight the impact work environments and working conditions have on mental health. As well as the strategic plans needed to address the root cause of some of the workplace issues highlighted, we believe that there is an immediate need for employers to consider what they can do to support positive wellbeing. We plan to support this during 2023 by providing tools, training and support for pharmacy leaders that we hope will assist in embedding positive wellbeing practices into the workplace.”
Workforce planning for pharmacy urgently needed
As winter pressures mount, the RPS is calling for workforce planning for pharmacy to address skill mix and staffing levels so that workloads can be effectively managed.
RPS President Professor Claire Anderson said:
“The work environment and working conditions have a huge impact on mental health. With pharmacy teams at risk of burnout, governments urgently need to improve workforce planning for pharmacy that addresses head-on the issues of skill mix and adequate staffing which are at the heart of overload in pharmacy.
“The recruitment and retention of pharmacists and their teams is crucial if the ambitions for pharmacy to play a key role in the future NHS are to be delivered. Planning must be backed by long-term investment and training from both employers and governments to make work more rewarding and improve career pathways.
“A key plank of plans to provide better care for patients is to increase the number of pharmacists who train to become independent prescribers to benefit patients. This initiative can only work if it is underpinned by protected learning time rather than expecting people to undertake professional development at the end of a long working day, which is totally unacceptable.
“We look forward to working with stakeholders and governments to inform workforce planning for pharmacy which is also a common theme in the RPS visions for pharmacy across England, Scotland and Wales.”
Click here to view the full 2022 Workforce Wellbeing Survey report
The fourth annual workforce wellbeing survey for pharmacy was carried out from 20 September to 14 October 2022. There were 1,496 respondents, the majority being in practice between 11-39 years. The survey was open to both RPS members and non-members.